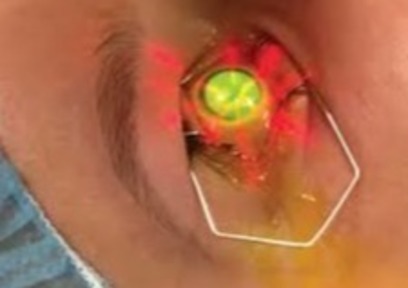
How Long Does CXL Last?

KC and Middle-Age
June 12, 2023
Side Effects & Complications of Crosslinking
July 6, 2023Originally published in NKCF Update (March 2023).
One frequent question from individuals considering corneal crosslinking (CXL) is “How long does it last?”.
The procedure that is recommended to halt or prevent corneal thinning and bulging and accompanying changes to vision was first described in 2003. Doctors at Carl Gustav Carus Hospital in Dresden, Germany reported that a combination of ultraviolet light and riboflavin eyedrops stopped keratoconus progression. Fifteen-year results of the initial cohort of patients was recently published. This represents the longest time period that individuals who undergo CXL have been monitored, and the results are informative.
Patients who had mild, moderate, or severe keratoconus were crosslinked between 2001 and 2006 using the Dresden Protocol, the epi-off method that is the basis for the FDA-approved treatment in the US. The mean age of these patients at time of treatment was 26 years old. Three years after treatment, the doctors reported that CXL was largely effective, with 92.5% success in stopping disease progression.
Now, fifteen years after treatment, 42 crosslinked eyes were examined and retested. The vision for 28 of 42 eyes (67%) was stable or better than 15 years previously. Corneal thickness and corneal steepness were also improved over the baseline results.
 Six eyes (14%) required retreatment. Retreatment is a repeat of the CXL protocol with ultraviolet light and riboflavin drops. One eye was retreated nine months after the initial CXL. The remaining five began to show signs of increased corneal steepening after many years. One patient was retreated 7 years after the original CXL, two patients at year 11, and two at year 12. All patients who experienced treatment failure had severe keratoconus or suffered from allergies or inflammatory disease.
Six eyes (14%) required retreatment. Retreatment is a repeat of the CXL protocol with ultraviolet light and riboflavin drops. One eye was retreated nine months after the initial CXL. The remaining five began to show signs of increased corneal steepening after many years. One patient was retreated 7 years after the original CXL, two patients at year 11, and two at year 12. All patients who experienced treatment failure had severe keratoconus or suffered from allergies or inflammatory disease.
In cases where a second treatment was necessary, disease progression was halted. No patients required a corneal transplant or a third CXL treatment.
No serious complications resulting from crosslinking were reported. Mild corneal scarring was detected in 36% of the patients (15 of 42 eyes), but these scars did not affect their vision.
These results should be useful to patients considering CXL for progressive keratoconus. In the majority of cases, the Dresden protocol results in stable cornea curvature and stable vision. However, the procedure is not a ‘one and done’ for everyone. Doctors should continue to monitor patients for changes that suggest a retreatment is recommended. This is especially true for patients with severe keratoconus or who continue to rub their eyes because of allergies or habit.
Reference: Corneal crosslinking with riboflavin and UVA light in progressive keratoconus: Fifteen-year results, Raiskup F, Herber R, Lenk J, et al, Am J Ophthalmol, Jan 31, Online ahead of print, 2023