Keratoconus and Down syndrome
The Need to Know About Keratoconus
Infants born with Down syndrome (DS) face a multitude of health issues, among them eye and vision disorders. For instance, the majority of children with DS have refractive errors, so it is probable that your child will be prescribed eyeglasses. Other common eye disorders like lazy eye (amblyopia) or crossed eyes (strabismus) can be diagnosed early and treated. Doctors estimate that between 5-30% of children with DS also have an irregular cornea or keratoconus (KC).
Like other vision problems, KC can affect an individual’s ability to function at the highest level possible. Poor vision may increase social isolation and make performing daily activities difficult. Children with DS may not complain about their vision until permanent changes have occurred. For that reason, it is important for family members to watch for signs of deteriorating vision and to schedule regular eye exams.
About Keratoconus
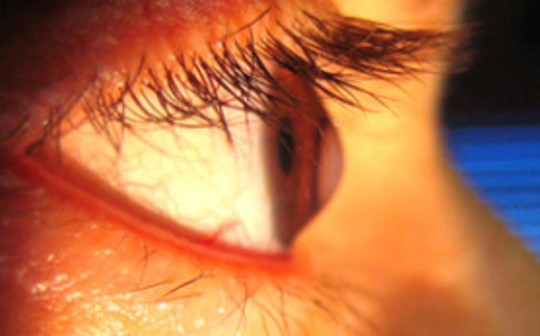 The cornea is the clear, round and spherical front of the eye. A normal cornea is only as thick as 3 pieces of copier paper. Keratoconus causes the cornea to become even thinner. As the disease progresses, the cornea stretches and may scar or form a cone-shaped bulge. When the cornea is no longer round and spherical, images are distorted. While KC will not result in blindness, some common complaints include glare, haze, and blurred or double vision, and it becomes harder to function as the disease progresses (gets worse).
The cornea is the clear, round and spherical front of the eye. A normal cornea is only as thick as 3 pieces of copier paper. Keratoconus causes the cornea to become even thinner. As the disease progresses, the cornea stretches and may scar or form a cone-shaped bulge. When the cornea is no longer round and spherical, images are distorted. While KC will not result in blindness, some common complaints include glare, haze, and blurred or double vision, and it becomes harder to function as the disease progresses (gets worse).
KC affects both sexes, and is a bilateral (both eyes) disease, although one eye may be more affected than the other. Changes to the cornea as a result of KC usually become evident during adolescent or teen years, and can progress significantly over the next few decades. There is some evidence that puberty sets off some of the changes associated with KC. Children with DS have corneas that are thinner and steeper than the general population, so even children who are not diagnosed with KC may have some of the same vision complaints and should be evaluated. The important indicator of KC is that the cornea continues to weaken and change shape.
Make a Plan with your Eye Doctor
While severe KC may result in changes to the eye that are visible to the public (a cone-shape when viewing the eye from the side), the goal is early diagnosis and treatment. It is important to find an eye doctor who can identify signs of keratoconus in patients with DS. Measuring vision using the standard letter or picture chart may not distinguish between healthy eyes and early keratoconus. Beginning in adolescence, appropriate eyecare for those with DS means having regular topography scans to compare the shape of the cornea to previous results. It will likely take more than one visit to determine if there are changes consistent with KC. Patient participation and cooperation for these tests is paramount. Since even the slightest change has serious consequences, the doctor may need to repeat the test several times in a single visit to get a reliable reading. If your doctor diagnoses your child with KC, your goal should be to stop the progression of KC via crosslinking, and to get the best possible vision for your child.
Corneal Crosslinking
Crosslinking (CXL) is a one-time treatment than stiffens the collagen in the cornea and results in slowing or stopping the progression of KC. Early detection and treatment prevents further vision deterioration and avoids the likelihood of a corneal transplant in extreme cases.
CXL is an FDA-approved procedure using ultraviolet light and eyedrops containing vitamin B (riboflavin). The procedure takes about an hour and is normally performed in a doctor’s office. Patients must be able to follow directions during the treatment and focus on the ultraviolet light during the procedure. If you do not believe your child can cooperate during the treatment, your doctor may elect to perform CXL under anesthesia and may treat both eyes at one time. Your doctor may recommend a modified version of CXL that does not require removal of the epithelium, the outermost portion of the cornea which is done to assure the eyedrops saturate the cornea.
In the majority of cases, CXL halts the progression of KC, but you should continue to have your child’s vision monitored after CXL with regular eye exams and testing to detect any changes to the cornea.
Eyeglasses or Contact Lenses for Vision Correction
In addition to treating KC, patients must also be offered the opportunity for improved vision. In the early and mildest form, KC can be managed with eyeglasses. While the vision correction with eyeglasses is not optimal, spectacles provide functional vision and are the best alternative for many with DS. As keratoconus progresses, eyeglasses can no longer accommodate for the irregular cornea and the best option is contact lenses. Contact lenses come with a new set of challenges for both caregivers and patients. The process of wearing, cleaning and caring for contacts requires healthy habits and a high level of responsibility. For many with DS, contact lenses can be a successful option. Your doctor can advise you on options. Neither eyeglasses nor contact lenses will stop the progression of KC. Without crosslinking, your child’s need for vision correction may need to be adjusted regularly.
Corneal Transplant
In a small minority of cases, doctors will recommend a corneal transplant for patients with KC. The scarred and misshapen cornea is replaced with a donor cornea. Any patient who undergoes a corneal transplant will need to be closely monitored in order to avoid complications. The outcome for individuals with DS who receive a corneal transplant is variable and depends greatly on patient compliance.
A Final Word about Eye Rubbing
Keratoconus is strongly associated with eye rubbing. Patients are encouraged to avoid eye rubbing as it can cause additional damage to already weak corneas. The majority of patients with KC rub their eyes and many are not even conscious of their behavior. Some eye rubbing may be related to ocular allergies; your doctor can recommend over-the-counter or prescription eyedrops that can provide relief for itchy eyes. In any event, it is important for family members to call attention and help break this habit.
Takeaway points for families affected by Down syndrome:
- Keratoconus (KC) is a bilateral progressive eye disease that causes the corneas to become weak and change shape, resulting in serious vision problems.
- In general, individuals with DS have corneas that are thinner, less rounded and more steep than the general population. Up to 30% of individuals with DS may have keratoconus.
- If there are ongoing changes to the cornea, crosslinking (CXL) is the FDA-approved treatment that can slow or stop KC. There is no cure for KC.
- Vision correction in the form of eyeglasses or contact lenses may improve quality of life and ability to perform independently.
- All individuals with keratoconus should make every effort to avoid eye rubbing.
- It is important to find eyecare professionals familiar with the unique vision problems of children with DS and who are experienced in caring for them.
Free Down Syndrome and Keratoconus Pamphlet and Patient Guide
 This pamphlet includes specific information about Down syndrome and keratoconus and will be sent when NKCF mails the 22-page, full color brochure, the Keratoconus Patient Guide. The Guide offers updated information about causes and treatments for keratoconus. These booklets are especially useful for newly-diagnosed patients and their family members and friends.
This pamphlet includes specific information about Down syndrome and keratoconus and will be sent when NKCF mails the 22-page, full color brochure, the Keratoconus Patient Guide. The Guide offers updated information about causes and treatments for keratoconus. These booklets are especially useful for newly-diagnosed patients and their family members and friends.
To receive your free copy of the Keratoconus Patient Guide and Down Syndrome & Keratoconus bifold, fill out the form below. You will be automatically receive Update, the NKCF quarterly newsletter as well as invitations to participate in free education webinars and conferences.
* If you are accessing this form through a smart phone, please turn your device from upright (vertical) to landscape to fully access order form.

